From the Journal: Biomicrofluidics
WASHINGTON, May 5, 2022 – Lymphedema often occurs in survivors of breast cancer, because they are at high risk for lymph node damage or removal during surgical procedures. The locations of these nodes often make fluid and proteins collect in the arm, so treatment consists of compression sleeves that seek to restore normal flow. However, current techniques are expensive and inconvenient.
In Biomicrofluidics, by AIP Publishing, researchers from the University of Waterloo’s Microfluidics Laboratory and DIESEL Biomechanics Laboratory, Breast Rehab, and Myant, Inc. developed a soft robotic sleeve controlled with a microfluidic chip that reduces treatment cost, weight, and power consumption. The prototype is more portable than previous devices, and the underlying mechanisms can extend to other treatments, such as prosthetics.
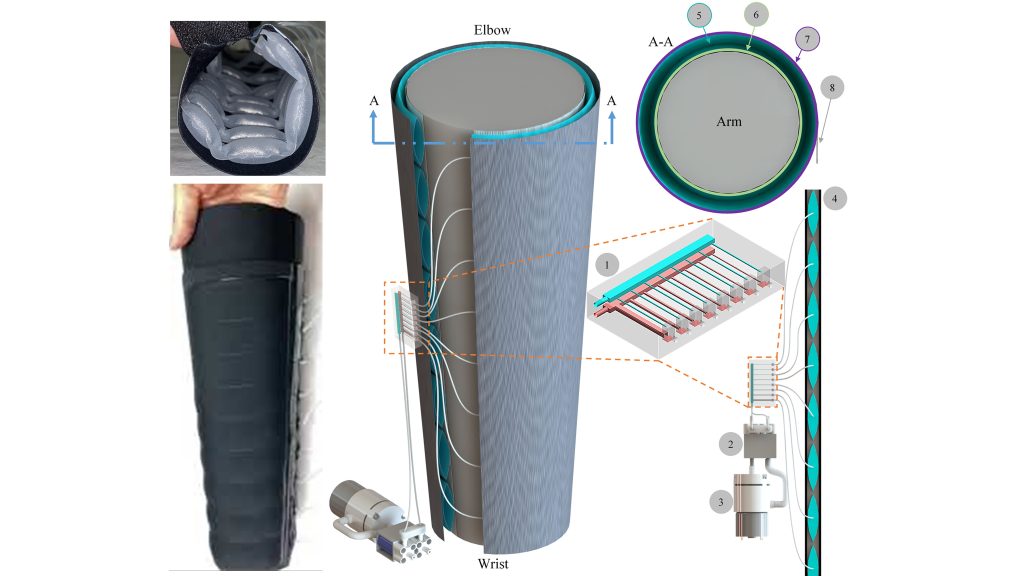
The microfluidic chip has 16 channels, each acting as a sort of pipeline. Just as pipelines with different diameters create different flow speeds, the channels each have a different resistance. The differing resistances create a time delay between the flow through each channel, causing balloons in the sleeve to sequentially inflate and push fluid upwards, out of the arm.
The design requires only two miniature valves, which take the place of eight bulky, energy-consuming valves. As a result, the cost is cut from thousands to hundreds of dollars. It operates using a 3.7-volt lithium-ion battery within a control box weighing less than an iPhone 13, in contrast to previous technology that required a wall outlet.
“My definition of wearable is you can wear it and do whatever you want, and not be plugged into a wall,” said author Carolyn Ren. “Bringing in the microfluidics field, we wanted to make the system battery-powered but without compromising the performance.”
By placing a sensor between the sleeve prototype and the arm, the team measured and optimized the sleeve pressure to encourage fluid flow.
The researchers are currently recruiting for patient testing. They intend to use their device patent to develop a commercially viable product.
Microfluidic chips could also be incorporated into prosthetics for lower leg amputees.
Pressure is unevenly distributed around the leg during walking, and the leg swells to change sizes throughout the day, but traditional prosthetic sockets cannot adjust accordingly. A balloon system like the lymphedema sleeve could apply the correct amount of pressure to the leg dynamically and inflate or deflate to change size on demand.
“We look at these problems from different angle, but I think there are a lot more things microfluidics can contribute to these areas,” said Ren.
###
For more information:
Larry Frum
media@aip.org
301-209-3090
Article Title
Authors
Run Ze Gao, Vivian Mai, Nicholas Levinski, Jacqueline Mary Kormylo, Robin Murdock, Clark Dickerson, and Carolyn Ren
Author Affiliations
University of Waterloo, Breast Rehab, Myant Inc.
