From the Journal: Biomicrofluidics
WASHINGTON, September 1, 2020 — Diagnostic devices that are used at home or in doctors’ offices are often not sensitive enough to detect small amounts of a virus that might be present in samples from asymptomatic patients, which can occur in early stage COVID-19. In Biomicrofluidics, by AIP Publishing, scientists report a membrane-based invention that can concentrate the virus content of a sample of urine or saliva, allowing it to be detected.
To increase sample concentration, previous groups have used gel particles, coupled to a chemical dye, to trap and detect a virus, but this approach is restricted to specific viruses that can bind to the dye. In addition, the testing time can be more than 30 minutes and requires expensive equipment.
Other approaches have been tried, but all lack the ability to diagnose different viruses or other biosubstances of interest, such as human chorionic gonadotropin, a hormone present in the urine during pregnancy.
Researchers at the University of Cincinnati and Wright-Patterson Air Force Base tried two different devices, both based on similar membrane-filter systems.
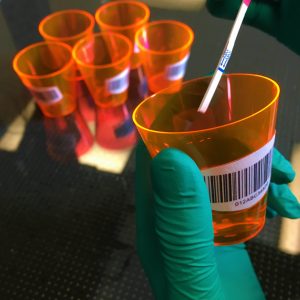
The first device was a fully integrated concentration unit coupled with a component that could detect the virus in question. A vacuum was used to pull water through the membrane, leaving behind the virus in a more concentrated solution, and the sample was analyzed in the same device.
“The amount of time needed to complete the concentration process was very slow,” said author Amy Drexelius. “On average, each device took about 30 minutes to complete the concentration process. We, therefore, concluded that the vacuum driven auto-staging device is not practically useful and turned to an alternate device utilizing a much higher positive pressure.”
The second device was considered because the investigators realized that by applying high pressure, instead of high vacuum, they could increase the pressure differential between the sample and the surroundings. A nitrogen gas tank and regulator were attached to their second device, allowing the application of up to 100 pounds per square inch of pressure.
The group investigated real biofluids, saliva and urine, spiked with samples of protein from influenza A virus. Other samples contained HCG.
“The test results were extremely consistent with the second device, showing a concentration result of 33 times that of the original sample,” said Drexelius. “Preconcentration of a 1-milliliter sample could be achieved in five minutes or even faster with higher applied pressures.”
The novel coronavirus that causes COVID-19 was not tested, but the method should work for it, since the technology could successfully detect influenza A. Both are respiratory viruses likely to be present in saliva. The technique is, in addition, promising for pregnancy testing, where early results are also highly desirable.
###
For more information:
Larry Frum
media@aip.org
301-209-3090
Article Title
Analysis of pressure-driven membrane preconcentration for point-of-care assays
Authors
Amy Drexelius, Anna Hoellrich, Andrew Jajack, Eliot Gomez, Michael Brothers, Saber Hussain, Steve S. Kim, and Jason Heikenfeld
Author Affiliations
University of Cincinnati and Wright-Patterson Air Force Base
