From the Journal: APL Bioengineering
WASHINGTON, June 9, 2020 — Benchtop tools for studying the respiratory system misrepresent the interdependence between the diaphragm, abdomen and lungs. Meanwhile, computational models often hide the mechanisms in a black box computation, without a clear picture of what transpires in the process.
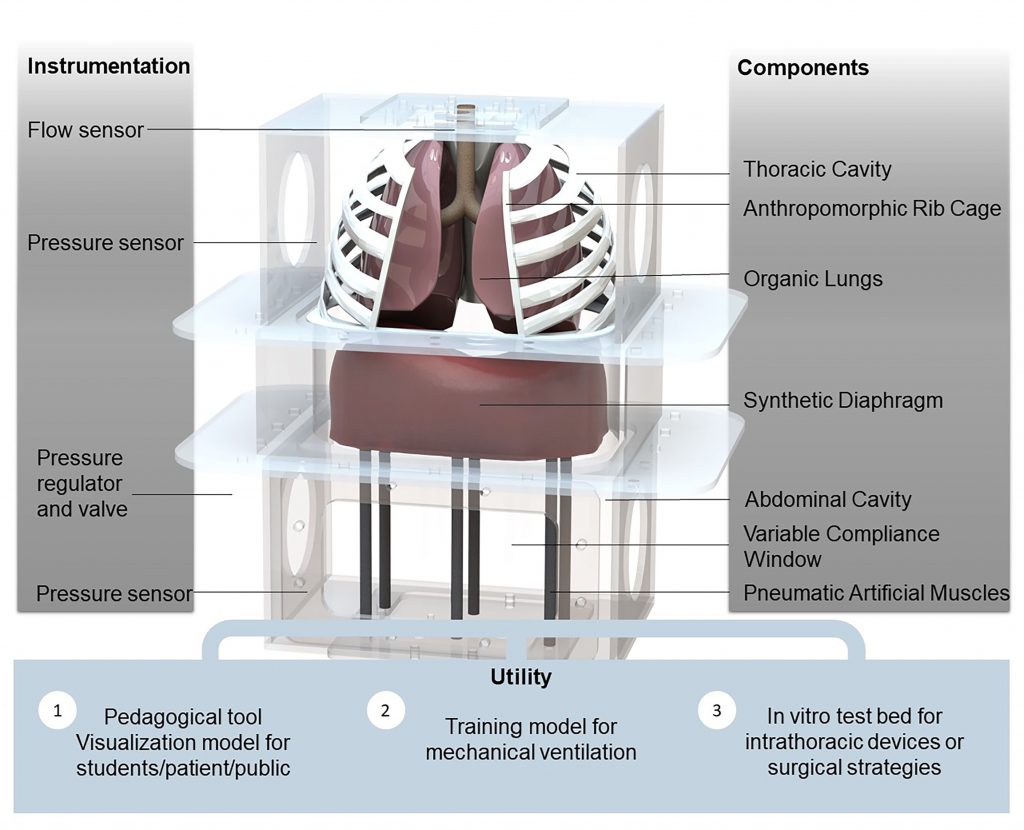
This means students form a poor understanding of respiratory mechanisms and makes it hard to train clinicians for real scenarios or prototype embeddable medical devices.
“If students can visualize pleural and abdominal pressure curves being generated in real time, while simultaneously observing diaphragm motion and lung inflation and deflation, it helps them establish an mental model, which can be called on and interrogated for different conditions, both physiological and pathological,” author Ellen Roche said.
In a paper published in APL Bioengineering, by AIP Publishing, Roche and co-authors created a high-fidelity respiratory simulator that accurately represents the interplay between the abdomen, diaphragm, lungs and pleural space, the fluid-filled membrane surrounding the thorax and lungs.
“We are excited about using synthetic actuators to actuate organic material, because we can preserve tissue structures while achieving reliable, tunable and deterministic motion with a soft robotic structure,” Roche said. “Our ultimate goal is to develop a model that combines the mechanics of the respiratory and cardiovascular systems to elucidate and characterize their interdependency and to test new therapeutic strategies.”
The model they created, using swine lungs, soft robotic materials and artificial muscles, allows precise tuning of pressure in each part of the system, so specific disease conditions can be tested to show how even minor changes affect overall respiratory function.
For example, the model was successfully used to test three types of pneumothorax, when air enters the pleural space, and obstructive lung disease by increasing flow resistance in the airway. The authors also tested a patch for repairing lung punctures and showed the system of sensors measuring flow, volume and pressure in the model is able to precisely measure airway pressure and pleural pressure.
The model, which is completely modular with parts that can be removed or replaced, also proved extremely useful for testing ventilator-only respiration by removing the elastomeric diaphragm.
“We are currently using it as a realistic testbed to test different ventilator options that have been developed for the COVID-19 pandemic,” Roche said.
The authors plan to add cardiovascular components to their model to further increase its usability to study complex problems involving respiratory and cardiovascular systems.
###
For more information:
Larry Frum
media@aip.org
301-209-3090
Article Title
An organosynthetic soft robotic respiratory simulator
Authors
Markus A. Horvath, Lucy Hu, Tanja Mueller, Jon Hochstein, Luca Rosalia, Kathryn A. Hibbert, Charles C. Hardin and Ellen T. Roche
Author Affiliations
Massachusetts Institute of Technology, Technische Universtat Munchen, Harvard University
